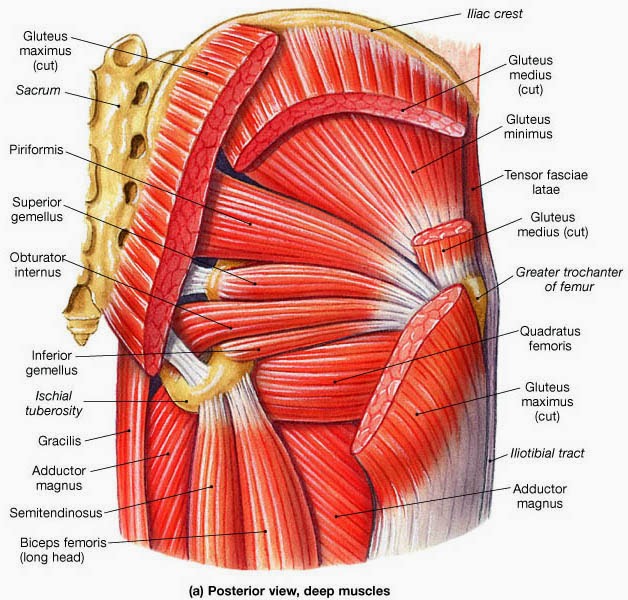
A balanced hip: Part I
The hip is a neatly designed joint, organized in a way to allow functional mobility, but still has proper constraints in place to maintain stability, including 3 ligaments (Nam et.al, 2011). These three ligaments are the ischiofemoral ligament, pubofemoral ligament, and iliofemoral ligament.
There are 6 deep muscles that stabilize the hip in the socket, followed by several layers of muscle that move the joint a variety of different directions, culminating with the gluteus maximus muscle which not only generates power and propels the body forward, but is also believed to be the point of load transfer from lower extremity to torso via the thoracolumbar fascia (Barker et.al. 2014). Directly opposing the lateral hip is the “groin” area. This area connects the abdomen and the lower limbs via the inguinal region, consisting of abdominal muscles (internal and external oblique, transverse abdominis, rectus abdominis, and the pyramidalis), the inguinal canal, and the femoral triangle (Valent et.al, 2012). During movement, the pubis symphysis is stabilized synergistically by the abdominals and the erector spinae, and the adductor muscles work in an opposing manner to provide stability to the area during load transfer. In the front of the hip are your “hip flexors,” which flex the femur in the sagittal plane. One of these muscles, the psoas, has attachment points on the lumbar vertebrae and is believed to play an important role in lumbar spine stability in an upright stance (Penning, 2000). It also shares fascial connections to the diaphragm and some believe it may play a role in overall trunk stability, along with the diaphragm, transverse abdominis, multifidus, and pelvis floor (Sajko & Stuber, 2009). A variety of issues can occur in and around the hip joint, including minor issues, such as tendon snapping, and more serious pathologies such as femoral acetabular impingement syndrome (Byrd, 2007). Interestingly, hip pathologies usually present as a “pain in the groin,” rather than pain in the more centralized hip joint area. Obviously, the cause for these pathologies are multi-faceted in nature, and it is worthwhile to note that the hip receives innervation from branches of L2-S1, with the L3 dermatome innervating much of the medial thigh, so if you or someone you work with has chronic groin pain, refer to an M.D. to rule out serious hip or lumbar spine pathology and make sure exercise is cleared.
Clearly, the hip and the muscles surrounding the hip play an important role in movement. It can be unclear how to train this area (do I focus on hip internal rotation or external rotation? Do I stretch the hip flexor or instead think about glute activation?) Each person is unique and what works for some might not work for all; however, hopefully we can begin to examine ways to move the body and integrate the hip in a balanced way. It is important to first bring awareness to the area and see if the hips are balanced, or if any asymmetries exist. An easy way to check this is to lie down on your back and begin noticing the weight of the pelvis on floor. As you begin thinking about this area, ask yourself if the weight of the pelvis on the floor feels even or if it feels unbalanced. If it feels unbalanced, ask yourself which side feels heavier against the floor. (If you have a difficult time identifying the contact of the pelvis with the floor, I strongly encourage you to work on some breathing exercises and learn how to engage your core using your breath. It is possible that by simply focusing on the sensation of your exhale, you will begin to feel a stronger sense of weight of the pelvis). If your pelvis feels like it isn’t quite balanced, chances are this asymmetry will be present during movement. Consider that your muscles are designed to work in a specific manner depending on their length-tension relationships. If you have a pelvic asymmetry, muscles on one side of the pelvis will be in a different position than the muscles on the other side of the pelvis. Unless you begin to correct the imbalance, your muscles will be working differently on the two sides. Now that you have assessed your pelvic position in a supine position, sit down on a bench or chair with your feet flat on the ground. Glance down at your feet. How did you naturally sit? Is one foot slightly in front of the other, or are your feet even? If your feet aren’t even, can you pull the hip of the foot that is forward back a touch to even out the feet? Now, notice the contact of your sitting bones on the bench. Are they both rooted evenly, or is one in better contact than the other? If you can’t find or feel either sitting bone, I highly recommend some breathing work with an emphasis on core integration (you might begin to notice a theme). If you feel one better than the other, can you begin to root the sitting bone that you can’t feel and then relax back to what feels “normal?” Do this a few times and relax. See if there is a difference. Now, come into a standing position. Once you are in a position that feels comfortable for you, glance down at your feet and see if they are even. If they aren’t, can you move the foot back that is forward with your hip? Now, take your hands on your hips and look down and see if one finger appears to be slightly forward or higher than the other, or if they look balanced. Observe the contact of your feet with the floor. Are your feet balanced on the floor, or are you standing more in your heels or toes? Where is your weight more loaded? Is it more on your left foot or your right, or is it even? Find balance. What happens when you spread your toes and lift your arch? Do your feel any activity in your hips? If you have a high arch, what happens when you engage the center of the foot and press the arch towards the floor? Do you feel any activity in your hips?
Before training the hips, it is important to understand there can be imbalances and asymmetries in our pelvis. This influences how we perform movements and which muscles are activated during movement. Bringing awareness to the area is often the first step in recognizing asymmetries that might exist. Asymmetries also affect the body’s ability to move in an efficient manner. Part II will focus more on actually training the hips and integrating the movement with the rest of the body.
Nam, D., Osabahr, D.C., Choi, D., Ranwat, A.S., Kelly, B.T., & Coleman, S.H., (2011). Defining the origins of the iliofemoral ischiofemoral, and pubofemoral ligaments of the hip capsuloligamentous complex utilizing computer navigation. HSS Journa, 7(3), 239-243.
Barker, P.J., Hapuarachchu, K.S., Ross, J.A., Sambaiew, S., Ranger, T.A., & Briggs, C.A., (2014). Anatomy and biomechanics of gluteus maximus and the thoracolumbar fascia at the sacroiliac joint. Clinical Anatomy, 27(2), pp. 234-240.
Valent, A., Frizziero, A., Bressan, S., Zanella, E., Giannotti, S., & Masiero, S., (2012). Insertional tendinopathy of the adductors and rectus abdominis in athletes: a review. Muscles, Ligaments and Tendons Journal, 2(2), 142-148.
Penning, L., (2000). Psoas muscle and lumbar spine stability: a concept uniting existing controversies. Critical review and hypothesis. European Spine Journal, 9(6), 577-585.
Sajko, S., & Stuber, K., (2009). Psoas Major: a case report and review of its anatomy, biomechanics, and clinical implication. Journal of Canadian Chiropractic Association, 53(4), 311-318.
Byrd, J.W.T., (2007). Evaluation of the hip: history and physical examination. North American Journal of Sports Physical Therapy 2(4), 231-240.